Infantile Hemangiomas
What Is an Infantile Hemangioma?
An infantile hemangioma (hee-man-jee-OH-muh) is a type of birthmark. It happens when a tangled group of blood vessels grows in or under a baby's skin. It’s usually noticed in the first few days to months of life. Most infantile hemangiomas grow larger at first, and then slowly go away. But some can leave a mark or loose skin.
What Are the Types of Infantile Hemangioma?
The two main types of infantile hemangioma are:
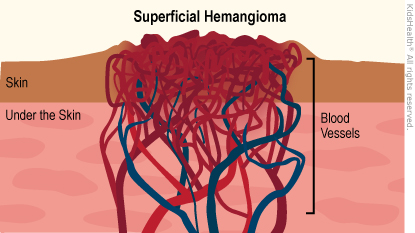
- Superficial hemangiomas, or cutaneous ("in-the-skin") hemangiomas, grow on the skin's surface. They're also called strawberry hemangiomas or strawberry marks because of their bumpy red appearance.
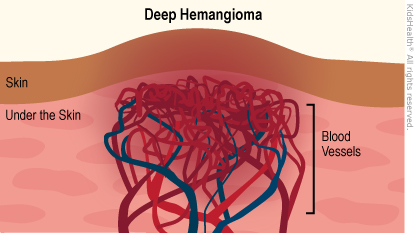
- Deep hemangiomas grow under the skin, making it bulge, often with a blue or purple tint. Deep hemangiomas are also called subcutaneous ("under the skin") hemangiomas.
Sometimes a hemangioma can be made up of both types.
Hemangiomas also may develop in organs inside the body, such as the kidneys, lungs, liver, or brain.
What Are the Signs & Symptoms of an Infantile Hemangioma?
A baby might have no sign of a hemangioma at birth or can have a flat blue or red patch. The infantile hemangioma grows over a few months. Later during the first year of life, it starts to shrink (or involute) until little or none of the tangled blood vessels remain. Shrinking continues until a child is age 7 or older.
Many infantile hemangiomas go away completely. But sometimes a hemangioma leaves behind an area of discolored or stretched skin.
What Problems Can Happen?
A hemangioma may cause problems by:
- blocking vision or eye movements
- reducing air flow through the nose and mouth
- bleeding
- breaking down the skin surface (ulceration)
- having enough blood flowing through it to put a strain on the baby's heart
- affecting the child's appearance
Infantile hemangiomas often grow on the head or neck, where they can't easily be covered by clothing. Sometimes, kids with a hemangioma get teased or bullied.
What Causes Infantile Hemangiomas?
Doctors don’t know what causes a hemangioma. It may be related to changing oxygen levels that happen while the baby is developing in the womb.
Hemangiomas are more common in babies born prematurely (before their due date), at a low birth weight, or as part of a multiple birth (twins, triplets, etc.). A child can have more than one hemangioma.
Hemangiomas may run in families, but no genetic cause has been found.
How Are Infantile Hemangiomas Diagnosed?
Doctors usually recognize an infantile hemangioma of the skin based on how it looks and when it appears. Tests typically aren't needed. If doctors need to see how far a hemangioma goes under the skin or if it affects any internal organs, they will do an MRI or ultrasound.
How Are Infantile Hemangiomas Treated?
Most infantile hemangiomas are not treated because they usually go away on their own.
Doctors treat hemangiomas that are very large, cause problems like bleeding or blocked vision, or affect someone’s appearance (for example, treatment can improve healing of a hemangioma on the face).
These treatments might be used alone or in combination:
- medicine:
- injected into the hemangioma
- taken by mouth or given into a vein (by IV line)
- surgery to remove the hemangioma
- surgery to fix the skin if it is loose after the hemangioma goes away
- tying the vessel shut in a surgical procedure (ligation)
- embolization: blocking the vessels from the inside using a long, thin tube called a catheter that reaches the hemangioma through blood vessels
- surface laser for skin color changes
Not all infantile hemangiomas need treatment. Talk with your doctor about the best plan for your child.
How Can Parents Help?
Other kids and adults may be curious about a child's hemangioma, especially one that is on the face. Help your child feel calm by having a simple response ready like, "It's just a birthmark. I was born with it.”
Talk openly with your child about their hemangioma. Tell them that in time it probably will go away. Work with teachers and school staff to ensure your child has a supportive learning environment free from bullying.
You also can find more information online at:
